Sleep apnea is a disorder that involves brief periods of not breathing when the individual enters deeper sleep stages. When breathing stops, the individual becomes short of oxygen and partially wakes up again, which causes them to resume breathing. However, these respiratory events disrupt deep sleep throughout the night, and this can cause daytime drowsiness, cognitive impairment, auto and work-related accidents, and increased blood pressure and risk of stroke and heart attack.
Continue ReadingCategory: Research
Relieving Phantom Limb Pain Using Virtual Reality
Many people who have lost a leg or arm experience a persistent sensation known as a “phantom limb”, which can be associated with debilitating pain. Current therapies fall short of bringing relief to most of these individuals, but recent research using virtual reality equipment is showing promise.
In this video, MRRI Associate Director Laurel Buxbaum, PsyD, explains the reearch and results so far.
Robotics and Neurostimulation in Stroke Rehab
 Research has shown that robotics and non-invasive brain stimulation both can improve recovery from central nervous system damage. Can that recovery be enhanced by combining the two techniques? In the latest episode of the MossRehab Conversations podcast, Dylan Edwards, PhD, discusses his research into both areas and what he is learning from using them together. Continue Reading
Research has shown that robotics and non-invasive brain stimulation both can improve recovery from central nervous system damage. Can that recovery be enhanced by combining the two techniques? In the latest episode of the MossRehab Conversations podcast, Dylan Edwards, PhD, discusses his research into both areas and what he is learning from using them together. Continue Reading
NIH Funding Renewed for MRRI Postdoctoral Training Program
Moss Rehabilitation Research Institute (MRRI) has been awarded a 5-year renewal on its NIH-funded training grant entitled, “Postdoctoral Training in Translational Neurorehabilitation Research.” The grant is directed by John Whyte, MD, PhD, co-founder and former director of MRRI.
This is the only rehabilitation-focused institutional training program currently funded by the National Center for Medical Rehabilitation Research (NCMRR). The program offers mentored research training to individuals who have recently completed their PhD or MD degrees and wish to pursue careers in research that focus on understanding and treating cognitive and motor impairments that result from neurologic injury or disease. Continue Reading
Dr. Buxbaum Featured on ASNR Podcast
 Laurel J. Buxbaum, PsyD, who is presenting the Viste Award Lecture at the American Society of Neurorehabilitation (ASNR) Annual Meeting in November, joined a podcast with other presenters to talk about the upcoming conference.
Laurel J. Buxbaum, PsyD, who is presenting the Viste Award Lecture at the American Society of Neurorehabilitation (ASNR) Annual Meeting in November, joined a podcast with other presenters to talk about the upcoming conference.
The podcast captures conversations with five leading neurorehabilitation researchers talking about their current research and new directions in the field. Continue Reading
Dylan Edwards Steps into Role as MRRI Director
 Dylan Edwards, PhD, MRRI’s new director, has big visions for the institute’s future—which he sees as being just as bright as its prestigious past. Taking over for retiring director and co-founder John Whyte, MD, PhD, Edwards comes to MRRI from the Weill Cornell Medicine-affiliated Burke Neurological Institute in White Plains, NY. Dr. Edwards’ research has primarily focused on non-invasive brain stimulation and the use of robotics in recovery from stroke and spinal cord injury. At MRRI, he’ll find ways to continue his research while helping steer MRRI to new heights in the coming years. Continue Reading
Dylan Edwards, PhD, MRRI’s new director, has big visions for the institute’s future—which he sees as being just as bright as its prestigious past. Taking over for retiring director and co-founder John Whyte, MD, PhD, Edwards comes to MRRI from the Weill Cornell Medicine-affiliated Burke Neurological Institute in White Plains, NY. Dr. Edwards’ research has primarily focused on non-invasive brain stimulation and the use of robotics in recovery from stroke and spinal cord injury. At MRRI, he’ll find ways to continue his research while helping steer MRRI to new heights in the coming years. Continue Reading
Participants Needed for Virtual Reality Research Study
MRRI is looking for people with below-the-knee leg amputation(s) and phantom limb pain to participate in a virtual reality research study.
The study requires approximately two 90 minute visits per week for about six weeks. You will be paid $25 for each visit. Some reimbursement for transportation is available. Continue Reading
Understanding How People Plan and Execute Skilled Movements
Aaron L. Wong, PhD, an institute scientist at the Moss Rehabilitation Research Institute, studies how people gain the ability to perform skilled actions – the movements exhibited, for example, by professional athletes, dancers and musicians – as a model for how individuals might recover movement abilities following neurological disorders or stroke.
In this video, he discusses his research using a robotic arm to understand how motivation in the form of reward can be used to help people more efficiently reduce their movement errors.
Continue Reading
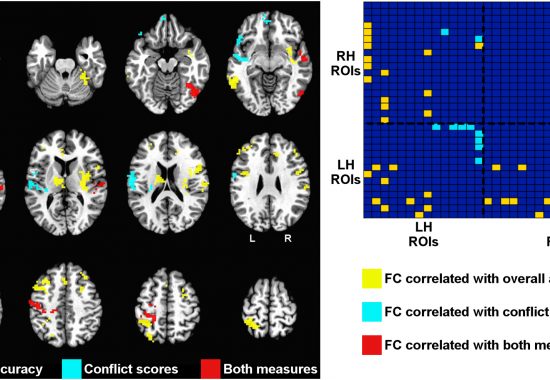
Functional Connectivity Predicts Complex Action Deficits After Stroke
MRRI Associate Director Laurel Buxbaum, PsyD, and colleagues from MRRI and the National Institutes of Health published the results of a new study showing that abnormalities in the connections between different brain regions determine clinical symptoms.
Studying How Left and Right Sides of Brain Affect Language
The core focus behind the work of Edward W. Wlotko, PhD, director of MRRI’s Cognitive Neurophysiology and Neuropsychology Lab is an examination of how the brain is able to understand language. He is particularly interested in uncovering how the two cerebral hemispheres each distinctly and jointly contribute to language processing. In this video, Dr. Wlotko describe his current research into the way hemispheric contributions to language processing may differ across individuals, with and without neuropsychological injury or disorder.